Bone Density Scan (DEXA)
Overview
Urology Associates offers a comprehensive Bone Density Study Department, complete with a full-size imaging table and a specifically trained professional to perform the exams.
Bone density measurement is used to determine the amount of mineral and calcium in your bones. The most commonly used test is Dual Energy X-ray Absorptiometry (DEXA). This involves lying on a table for 10-20 minutes while a low-dose x-ray beam scans your spine, hip, or both. There is no discomfort and no known risk from this diagnostic procedure, other than minimal radiation exposure.
Bone Density Scan FAQ
What is a Bone Density Scan (DEXA)?
Bone density scanning, also called dual-energy x-ray absorptiometry (DXA or DEXA) or bone densitometry, is an enhanced form of x-ray technology that is used to measure bone loss. DEXA is today’s established standard for measuring bone mineral density (BMD).
DEXA is most often performed on the lower spine and hips. Portable DEXA devices, including some that use ultrasound waves rather than x-rays, measure the wrist, fingers or heel and are sometimes used for screening purposes.
Why is a Bone Density Scan Done in Urology?
Major treatment options for prostate cancer include surgery, radiation, hormonal therapy, chemotherapy, and watchful waiting. Bone densities are done for patients that decide to go with hormone therapy to treat their prostate cancer and the effect it can have on your bones.
Testosterone is a male hormone produced primarily by the testicles. Testosterone can stimulate the growth of hormone dependent prostate cancer. As long as the body produces testosterone, prostate cancer will continue to spread. There are various types of hormonal therapies. The most common are:
- Drugs that reduce testosterone production by the testicles (i.e., LH-RH agonists).
- Surgical removal of the testicles (orchiectomy), which produce male hormones.
- Antiandrogen therapy to block the effects of testosterone.
Lupron, Zoladex, Eligard and Trelstar are types of hormonal therapy injections that many of our patients decide to use as their treatment option for prostate cancer. These LH-RH agonist drugs are used to shut down testosterone produced by the testicles. This decrease in testosterone can lead to other potential symptoms such as loss of Bone Mineral Density (BMD), which can eventually lead to osteoporosis.
A decrease or loss of testosterone affects bone regeneration, leading to bone weakness. Throughout our lives, our bones change, constantly renewing itself through a process called remodeling. In doing so, cells called osteoclasts break apart old areas of bone, and other cells called osteoblasts create new bone to fill in old areas. When this process is balanced, bone strength and bone health are maintained. When this process is not balanced, we start to see bone weakness. Many of our urologists will monitor your bone mineral density on an annual basis if you decide to have hormonal therapy for prostate cancer to make sure it does not start to give you bone weakness.
How is the procedure performed?
The DEXA machine sends a thin, invisible beam of low-dose x-rays with two distinct energy peaks through the bones being examined. One peak is absorbed mainly by soft tissue and the other by bone. The soft tissue amount can be subtracted from the total and what remains is a patient’s bone mineral density.
DEXA machines feature special software that compute and display the bone density measurements on a computer monitor.
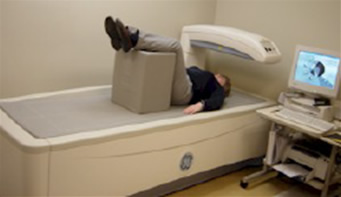
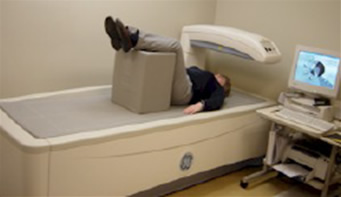
The DEXA examination measures bone density in the hip and spine, and the patient lies on a padded table. An x-ray generator is located below the patient and an imaging device, or detector, is positioned above.
To assess the spine, the patient’s legs are supported on a padded box to flatten the pelvis and lower (lumbar) spine (as seen below). To assess the hip, the patient’s foot is placed in a brace that rotates the hip inward. In both cases, the detector is slowly passed over the area, generating images on a computer monitor.
The patient must hold very still and may be asked to keep from breathing for a few seconds while the x-ray picture is taken to reduce the possibility of a blurred image. The technologist will walk behind a wall or into the next room to activate the x-ray machine.
How do I get my results?
A test report is produced from the computer that is attached to the bone density machine. Often, you will be scanned and seen by your urologist immediately after your scan. Some of our urologists will bring you back on another day to discuss the results.
Your test results will be in the form of two scores:
T Score
This number shows the amount of bone you have compared with a young adult of the same gender with peak bone mass. A score above -1 is considered normal. A score between -1 and -2.5 is classified as osteopenia, the first stage of bone loss. A score below -2.5 is defined as osteoporosis. The T score is used to estimate your risk of developing a fracture.
Z score
This number reflects the amount of bone you have compared with other people in your age group and of the same size and gender. If this score is unusually high or low, it may indicate a need for further medical tests.